If you have non-small cell lung cancer (NSCLC) and your doctor said your cancer is KRAS positive (which means you have this biomarker), we will help you understand what this means and how it impacts your treatment options.
This will help you talk with your doctor to decide the best treatment options for you.
What is a biomarker?
A biomarker is a substance that doctors can measure in tissue, blood, or other body fluids, like spit. Biomarkers are changes in a cell’s genes (parts of DNA) or proteins that cause the cancer to grow. These mutations are called “driver mutations” because they cause (or “drive”) cancer growth.
What is the KRAS biomarker in NSCLC?
The KRAS (pronounced K-raz) biomarker is a mutation (change or error) in the KRAS gene that causes cancer cells to grow. It stands for Kirsten RAt Sarcoma. In healthy cells, KRAS sends signals that tell the cell to grow. When mutated, KRAS causes too many signals and cells grow out of control, which causes cancer. You may hear doctors call it “KRAS-mutant lung cancer” or “KRAS-positive lung cancer.”
Normal KRAS sends signals in the cell that lead to healthy cell growth, which means one cell divides to become two cells.
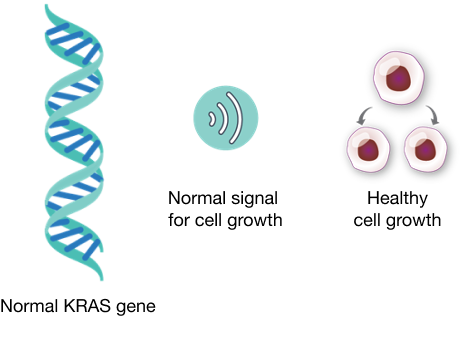
Mutated KRAS sends too many signals in the cell that lead cells to grow out of control, which means one cell divides into many cells.
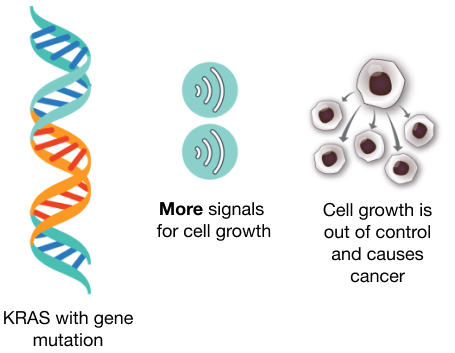
Types of KRAS mutations
There are many types of KRAS mutations. Each mutation is named based on the location of the error in the DNA.
About half of patients with a KRAS mutation have a type called KRAS G12C. The other types that are know to happen include:
- G12V
- G12F/D
- G13X
- Q61X
- G12A
What causes a KRAS mutation and who is most likely to have it?
KRAS mutations are acquired, which means they happen during your life. They are not passed down from your parents, and current research suggests you won’t pass them to your children.
Approximately 25%-30% of patients with NSCLC have a KRAS mutation. KRAS mutations are more likely to happen if you:
- Are of Western European descent
- Have a history of tobacco exposure
- Have a history of asbestos exposure
How do I know if I have a KRAS mutation?
After being diagnosed with lung cancer, ask your doctor for comprehensive biomarker testing.
Comprehensive biomarker testing (also called comprehensive genomic profiling or molecular testing) checks your lung cancer for a full list of biomarkers that doctors have linked to NSCLC. It is important to know if you have any other biomarkers (in addition to KRAS mutations) to help decide what your treatment options might be. Some treatments work better on cancers with certain biomarkers.
The first step in biomarker testing is for your doctor to do a biopsy to take a sample of tissue from your lung cancer. The medical team will look at it under a microscope and test it to check for biomarkers. Make sure your medical team is using an FDA-approved biomarker test.
Learn more about biomarker testing and types of biopsies
How do doctors treat NSCLC with KRAS mutations?

You will work with your doctor to decide on the treatment that is best for you, based on your type and stage of NSCLC and your biomarkers.
Until recently, the standard (usual) first treatment for patients with KRAS-positive lung cancer was chemotherapy. In 2021, the FDA approved the first targeted therapy for NSCLC with KRAS mutations. In 2022, a second targeted therapy was approved for treating NSCLC with KRAS mutations in patients who have already had at least one cancer treatment.
- Sotorasib (Lumakras™): Approved for the treatment of adult patients with KRAS G12C-mutated locally advanced or metastatic non-small cell lung cancer (NSCLC), as determined by an FDA-approved test, who have received at least one prior systemic therapy.
- Adagrasib (Krazati™): Approved for the treatment of adult patients with KRAS G12C–mutated locally advanced or metastatic non–small cell lung cancer, as determined by an FDA-approved test, who have received at least one prior systemic therapy.
Research is happening quickly to test other types of treatments, which may change your treatment options. Your treatment options may include:
Targeted therapy
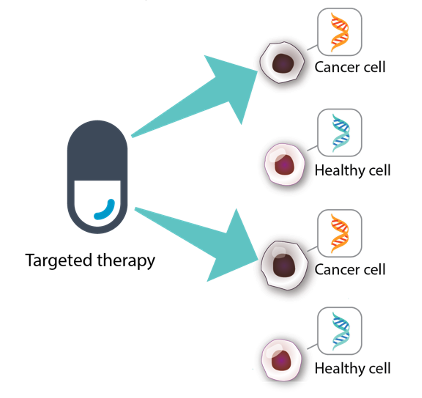
Targeted therapy is a type of treatment that finds and attacks certain parts of cancer cells and the signals sent to cancer cells that cause them to grow uncontrolled. They prevent the growth of cancer cells only, and do not harm healthy cells.
A targeted therapy works to control a specific biomarker, so it can only treat patients with that biomarker. There are currently two FDA-approved drugs for KRAS G12C-positive lung cancer. More treatments are being studied in clinical trials, including options for treating other types of KRAS mutations.
Targeted therapy attacks only cancer cells and leaves healthy cells alone.
Immunotherapy
Immunotherapy is a type of treatment that helps your immune system find and attack lung cancer. It is already a standard of care treatment for patients with NSCLC.
Many of the FDA-approved immunotherapies target another type of biomarker called PD-1/PD-L1. Because research has found PD-L1 biomarkers along with KRAS mutations in patient tumor samples, some clinical trials are now studying whether immunotherapy works to treat different types of KRAS mutations. Other clinical trials are testing a combination of KRAS G12C targeted therapy with immunotherapy. However, it is important to wait for biomarker testing results before starting treatment for NSCLC because, in some cases, it can be harmful to start immunotherapy if driver mutations are present.
Clinical trials
Talk with your doctor about taking part in a clinical trial for a new, possible treatment. Clinical trials are an important option for people with KRAS-mutated NSCLC because these trials offer access to the newest treatment approaches, which are not available otherwise because they are still being tested.
For example, researchers are currently testing cancer vaccines and lab-made immune system cells (cells that find and attack cancer) that will target KRAS-mutated NSCLC.
Cancer vaccines that treat existing cancer work to boost your body’s immune system to fight cancer. They may stop a tumor from growing or spreading or destroy cancer cells in the body.
Talk with your doctor
Talk with your doctor to understand your KRAS mutation and type of cancer, and to make a treatment plan together. Bring a pen and paper or use your cell phone to write down your questions and your doctor’s answers. You might start with these questions:
- Which type of KRAS mutation do I have?
- Did I have FDA-approved comprehensive biomarker testing – which biomarkers did you check for? If not, can you order it?
- What are my treatment options?
- Do I qualify for a clinical trial testing a new treatment for KRAS mutations?
- Is immunotherapy an option for me?
- What are the possible side effects of these treatments?
- Do I have any other biomarkers that may change my treatment options?
Tip: Print these questions out and fill in the answers with your doctor. Having this sheet on hand can help you to remember the conversation and plan for any next steps.
Newly Diagnosed with KRAS-Positive Lung Cancer?
In this video, LUNGevity's Amy Moore, PhD, sits down with Mark Awad, MD, PhD, a thoracic oncologist at Dana-Farber Cancer Institute, to discuss KRAS-positive lung cancer and the questions newly diagnosed patients should ask their doctors. They discuss first-line treatment, biomarker testing, clinical trials, and drug resistance.

